 16 This assumes that the patient’s pain generator(s) is/are the z-joints and not another spondylotic spine component, such as the disc. Given the low correlation of radiographic spondylosis with axial low back pain, the only means for an accurate diagnosis of symptomatic lumbar spondylosis secondary to facet arthropathy is to perform controlled diagnostic blocks of the medial branch nerves that innervate the z-joints. It can also be helpful in identifying synovial cyst borders with implications for surgical vs percutaneous treatment. Large amounts of fluid within the z-joints may represent instability and/or infection, which would warrant further work up and/or treatment, but is beyond the scope of this article.ĬT is typically utilized when an MRI is unobtainable or if fracture is suspected. MRI is generally not needed for diagnosis of spondylosis, but it is useful for evaluating the soft tissues and neural elements within the spine, especially to rule out neuroforaminal stenosis in patients with concomitant leg pain. If present, patients should undergo flexion and extension radiographs to rule out instability of the spine. Lateral views are important to study sagittal alignment and the presence of spondylolisthesis. Plain radiographs are not sensitive for detecting early z-joint OA or spondylosis, but are highly accessible, and often used. However, as spondylosis on imaging does not constitute a cause for LBP, imaging is typically ordered to rule out other disorders. Lumbar spondylosis is visible on multiple imaging modalities, including plain radiographs, magnetic resonance imaging (MRI), and computed tomography (CT) studies. 11 These should typically be administered at every office visit for following the patient’s progression. There are several validated outcome measures for grading functional limitations, including the following: McGill Low Back Pain Scale, Oswestry Disability Index, and the Medical Outcomes Study 36-Item Short-Form Health Survey. 
10 By definition, lumbar spondylosis exhibits no neurologic deficits however, because of its association with conditions that can affect the neurologic function of the lower limbs, it is imperative to ask about weakness, balance, gait, and bowel/bladder function. 6,10 The pain tends to worsen with extension, rotation, and standing it is better with lying and L-spine flexion. Pain may refer unilaterally or bilaterally to the buttock, hip, groin, and thigh regions although, typically, it does not extend past the knee. However, in some patients with acute or gradual onset of LBP, LS is present and could potentially be a cause of the pain. Triple arthrodesis has poor long-term results in patients with progressive deformity and sensory impairment.As mentioned previously, LS is a radiographic finding that does not rely on clinical symptoms for diagnosis. Surgical options include soft-tissue and plantar fascia releases for a flexible deformity, osteotomy for a fixed deformity, and tendon transfers to restore muscle balance. Management goals are to obtain a plantigrade, mobile, pain-free, stable, motor-balanced foot. Standing radiographs of the feet and spine, magnetic resonance imaging, and electrodiagnostic studies may be useful. Physical examination should include the cavovarus block test, which assesses flexibility of the hindfoot deformity and can direct surgical treatment. Initially, the cavus deformity is flexible, but if left untreated, it becomes a fixed bony deformity. A calcaneocavus foot may be seen in poliomyelitis, spinal dysraphism, and peripheral neuropathy. 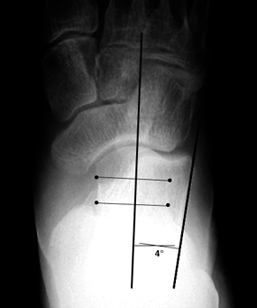
Common causes include progressive motor sensory conditions, typically Charcot-Marie-Tooth disease, and nonprogressive conditions such as cerebral palsy and poliomyelitis. Cavovarus, the most frequent type of cavus foot, presents with an elevated medial longitudinal arch, first ray plantar-flexion, and, if rigid, a fixed heel varus. A cavus deformity of the foot is easily recognizable, but appropriate neurologic assessment can help to determine the etiology. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
